How to Deal with Peripartum Depression: Symptoms and Treatment Options

Peripartum depression, also known as postpartum depression, is a common and severe condition that may develop during pregnancy or after childbirth. While having a baby is an exciting and joyous moment for most women, it may still cause anxiety in others.
As per the term “peripartum”, this type of depression often begins long before delivery. And it may last for some time after giving birth too. The good news is that this condition can be treated with the help of mental health practitioners, and treatment is especially effective if a diagnosis is made early.
If you think you experience depression symptoms during pregnancy or soon after childbirth, consult with our professionals to get help.
What Is Peripartum Depression?
Mental health experts describe this disorder as a mixture of major feelings that include fatigue, anxiety, extreme sadness, guilt, and indifference. Peripartum depression may also manifest itself in the changes in appetite, sleep, and energy, carrying some risks to the mother and unborn baby. Statistics show that approximately one in every seven women experiences this type of depression.
The definition also encompasses new fathers as they can exhibit signs of this major depressive disorder too. Their symptoms include fatigue and changes in sleeping or eating. Approximately 9% of fathers experience the condition within one year after the birth of their child. Fathers with a history of depression, young fathers, and those with financial challenges are at a higher risk of experiencing postpartum depression.
Peripartum Depression Symptoms
Pregnancy and the period following childbirth can be vulnerable to women. They often experience intense emotional, biological, social, and financial changes, putting them at a higher risk of developing mental health problems, primarily anxiety and depression.
According to the Diagnostic and Statistical Manual of Mental Disorder (DSM), the symptoms of peripartum depression include:
- Feelings of being a bad mother
- Prolonged feelings of sadness
- Trouble sleeping or sleeping too much
- Lack of interest in the baby
- Suicidal thoughts
- Difficulty thinking or making decisions
- Feeling worthless
- Increased restlessness
- Slowed movements or speech, observable by others
- Changes in appetite
- Fear of harming self or the baby
- Suicidal thoughts
The severity of the symptoms may change from time to time. Peripartum onset must have occurred during pregnancy or within four to six weeks after delivery for one to be diagnosed with it.
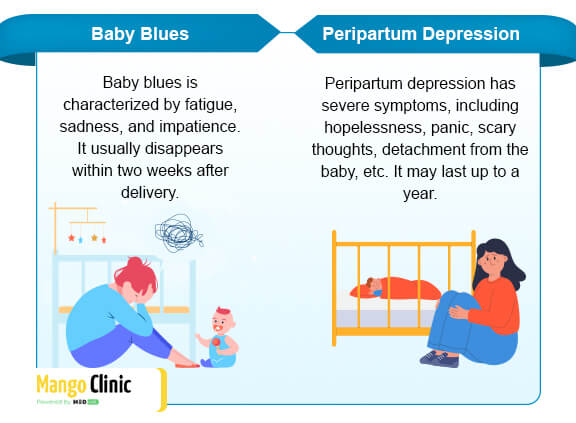
Baby Blues vs. Peripartum Depression
Most women experience baby blues in the days after child delivery. Symptoms include:
- Trouble sleeping
- Loss of appetite
- Crying spells
- Feeling overwhelmed, sad, or anxious
- Mood swings
The main difference is that baby blues symptoms usually disappear three to fourteen days after their onset. On the other hand, the effects of peripartum depression are prolonged as well as emotionally and physically draining and severe. That is why getting the proper diagnosis and treatment is crucial for the mother and baby.
Peripartum Depression: Causes
The most common cause of peripartum depression is hormonal changes. The levels of estrogen and progesterone are at the highest they can ever be during pregnancy. In the first 24 hours after childbirth, the hormones start to drop off to routine or where they were before pregnancy. Researchers think that these sudden hormonal changes after baby birth can cause depression.
The thyroid hormone levels may also drop after childbirth. The thyroid is a small gland in the neck that regulates the body’s use of and storage of energy. Low thyroid hormone levels may cause symptoms of depression. A simple blood test can help determine if this is the cause of the symptoms.
Other peripartum depression causes include:
- Feelings of being overwhelmed with the new baby
- Tiredness from inconsistent or lack of sleep
- Exhaustion from labor and delivery
- Stress from work and home duties
- Doubts about their ability to be a good mother
- Feelings of being less attractive
- Worrying about lack of free time
While these feelings are common in new mothers, peripartum depression is a depressive disorder. It requires immediate peripartum onset treatment. The condition isn’t a regular or expected part of being a new mother.
Self-diagnostics is not the case for postpartum depression—a person needs professional consultation to get suitable and effective treatment.
Peripartum Depression Diagnosis
While peripartum depression has existed for years, there isn’t a specific test to diagnose it. Healthcare providers often evaluate or assess the patient at their postpartum visit and discuss their health history and feelings since delivery. The standard assessment may include a pelvic exam, physical exam, and lab test. Many healthcare providers schedule a visit two to three weeks after delivery for screening across many risk factors that may point to depression.
No blood tests or body scans show a patient’s mood disorder. However, the doctor will ask specific questions about the state of mind, guided by these PPD screening tests:
- Edinburgh Prenatal Depression Scale (EPDS)
- 2-Question Patient Health Questionnaire (PHQ-2)
- 9-Question Patient Health Questionnaire (PHQ-9)
For any symptoms of depression that a patient displays, the doctor will continue with the assessment to evaluate the severity.
Peripartum Depression Treatment
Peripartum depression is a kind of depression treatable with counseling and medication. Also, getting enough rest, creating time for self, accepting help from family and friends, and connecting with other new mums can help improve the symptoms. Still, the most effective and common interventions in the line of treatment for postpartum depression are disclosed below.
Therapy
Also known as talk therapy or mental health counseling, psychotherapy helps the patient talk to a psychologist, psychiatrist, or other mental health specialists regarding their concerns or fears. Through therapy, they can find better ways to solve the problems they face, cope with their feelings, and respond to situations more healthily.
Antidepressants
The doctor may recommend antidepressants in the management of peripartum depression. Most types of these medications are safe for use during breastfeeding, posing little or no risk to the baby. Still, consulting with the doctor to weigh the benefits against the potential dangers of certain antidepressants is crucial.
Treatment for Severe Cases
When it’s a case of postpartum psychosis, there’s a need for immediate treatment at the hospital. Interventions to help manage the episodes include:
- Medication: This calls for a combination of mood stabilizers, antipsychotic drugs, and benzodiazepines to control the signs and symptoms. Also, Zulresso (brexanolone) injection can be used. This new medication has been recently approved by the FDA for the treatment of postpartum depression.
- Electroconvulsive Therapy: The treatment option is suitable for severe postpartum depression accompanied by postpartum psychosis. Doctors recommend it if the condition isn’t responsive to medication. They pass small electrical currents through the brain to trigger a brief seizure. The process changes the brain chemistry to reduce depression and psychosis symptoms.
Coping with Peripartum Depression
Feeling overwhelmed during and after pregnancy is a common thing, but sinking into depression is not something normal. If you experience unpleasant symptoms, seek professional help and talk to a psychiatrist. In a safe environment, you can trust the doctor to tell how you feel, learn how to find time for self-care, eat healthily, and master other beneficial methods of improving your mental state. Getting medical attention is a factor that can help eliminate the symptoms and overcome the effects of depression; contact us today to know more.









